- Products
- New Products
- Featured Products
- Color and Print Themes
- Blood Pressure Measurement
- NIBP / Vital Sign Monitors
- Digital Aneroid Sphygmomanometers
- Palm Aneroid Sphygmomanometers
- Pocket Aneroid Sphygmomanometers
- Pro's Combo Sphygmomanometers
- Multicuff Sphygmomanometers
- Clock Aneroid Sphygmomanometers
- Mercury Sphygmomanometers
- Home Blood Pressure Measurement
- Adcuff +
- Gauges
- Bulb & Valves
- Disposable Cuffs
- Reusable Cuffs & Bladders
- Sphygmomanometer Accessories
- Sphygmomanometer Parts
- Caseware
- CPR / Airway
- EENT
- Instruments & Accessories
- Laryngoscopes
- Penlights
- Pulse Oximeters
- Stethoscopes
- Thermometry
- Vital Signs Monitors
- Solutions
- About ADC
- Learning Center
- Support
- Blog
- Contact
Regulatory Updates Redefine Pediatric Readiness for EMTs
Written By:
Julie Redlich, Marketing Associate
Posted On:
April 15, 2026
EMS agencies across the country are entering a new phase of preparedness.
Following a major regulatory update in October 2025, several states, including New York, have expanded and formalized pediatric equipment requirements for certified EMS agencies. These updates reflect a growing national focus on ensuring that providers are fully equipped to care for patients of all ages. For EMS teams, this marks an important shift. Pediatric readiness is no longer just encouraged, it’s expected.
Why Pediatric Preparedness Matters
Pediatric patients represent a meaningful portion of EMS calls, but they also present unique challenges. In New York alone 9–10% of all EMS responses involve pediatric patients, translating to approximately 270,000–300,000 children treated annually. Despite this volume, pediatric readiness has historically varied across agencies, particularly when it comes to equipment availability and standardization. This disparity is exactly what these updated requirements aim to address.
From Recommendation to Requirement
For years, organizations like the American Academy of Pediatrics (AAP), American College of Emergency Physicians (ACEP), and others have worked together to define what properly equipped ambulances should carry. These efforts resulted in a standardized national equipment list for ground ambulances, designed to ensure EMS providers have the tools needed to deliver appropriate care in the field. Now, states like New York, and at least six others, are moving beyond guidance into formal regulatory requirements.
What’s Included in the Updated Requirements?
The updated guidance emphasizes age-appropriate, readily available equipment across a wide range of categories. For pediatric care, that includes:
- Airway management tools (multiple sizes for infants through children)
- Oxygen delivery devices sized for pediatric patients
- Immobilization equipment for smaller bodies
- Length-based resuscitation tools
- And – critically – pulse oximetry with pediatric capability
Why Pulse Oximetry Plays a Critical Role
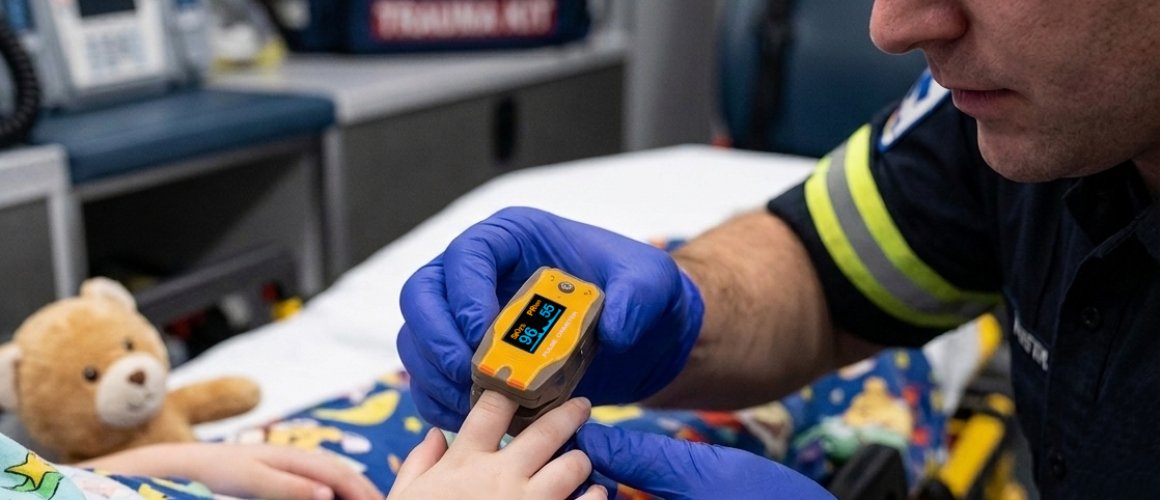
In pediatric emergencies, patient conditions can change quickly—and often without clear verbal communication. Pulse oximetry helps providers to detect hypoxia early and monitor oxygen saturation during transport, enabling them to make faster, more informed treatment decisions. And because pediatric patients require properly sized sensors and reliable readings, not all devices are created equal.
We’ve designed the Adimals 2150 Pediatric Pulse Oximeter specifically for pediatric patients, capable of delivering fast, accurate readings while being durable enough for prehospital environments and simple enough to use in high-pressure situations. Measuring both oxygen saturation and pulse rate, the Adimals 2150 has an SpO2 accuracy of ±2% and heart rate accuracy of ±2 BPM. With six changeable display modes, ten display brightness settings and no routine calibration or maintenance other than replacement of batteries, this pulse oximeter doesn’t just support compliance; it supports better care.
Meeting Requirements and Beyond
The October 2025 update reflects something bigger than regulation—it represents a continued commitment to improving outcomes for pediatric patients in emergency care. For EMS agencies, it’s an opportunity to evaluate current equipment, align with evolving standards and strengthen overall pediatric readiness. When it comes to treating children in emergency situations, preparation isn’t optional, it’s critical. At ADC, we design our products to go beyond the standard, delivering the reliability and precision EMS teams need when every second counts.
Sources:
